Development of autoimmune hepatitis in a psoriasis patient without immunosuppressive therapy
Article information
Abstract
We present a case of a 65-year-old man with psoriasis who developed autoimmune hepatitis (AIH) without receiving immunosuppressive therapy with either anti-tumor necrosis factor-α or methotrexate. The AIH had completely resolved at 2 months after prednisolone and azathioprine therapy. This case confirms the need to consider AIH in psoriasis patients who experience new elevations in liver enzymes. To our knowledge, this is first description of the development of AIH in an immunosuppressant-naïve patient with psoriasis.
INTRODUCTION
Psoriasis is a chronic autoimmune hyperproliferative skin disease of varying severity, affecting about 125 million patients worldwide, including approximately 2-3% of the general population in USA and Europe [1]. The typical psoriatic lesion is a well-demarcated erythematous plaque covered with silvery scales. The plaques may appear anywhere on the skin surface, but the mucosa is normally spared. T-cells play an important role in the development of psoriasis and produce cytokines, including interleukin-2 and tumor necrosis factor (TNF)-α, which are capable of inducing the inflammatory process and keratinocyte proliferation [2]. The three types of psoriasis treatment are topical therapies, phototherapies, and systemic therapies. The main systemic agents used for moderate to severe psoriasis are acitretin, cyclosporine, and methotrexate (MTX) [3]. The newer biologic agents, such as anti-TNF-α, used to treat severe to moderate psoriasis unresponsive to topical and systemic therapies, appear to have greater efficacy with less toxicity [3].
Autoimmune hepatitis (AIH) is chronic hepatitis of unknown etiology, which can progress to cirrhosis and is characterized by histological interface hepatitis, hypergammaglobulinemia, and circulating autoantibodies; it is commonly concurrent with autoimmune disease [4]. AIH is thought to be caused by environmental triggers that may have viral or drug etiologies, but most cases have unknown triggers [5]. There have been several reports of AIH developing in psoriasis patients treated with anti-TNF-α agents and MTX [6,7].
However, a literature review revealed no case reports of AIH in patients with psoriasis who did not undergo immunosuppressive therapy. Here, we describe a rare case of a 65-year-old male with an 8-year-history of psoriasis without immunosuppressive therapy, who was newly diagnosed with AIH.
CASE REPORT
A 65-year-old man with an 8-year-history of psoriasis was referred to our hospital with persistently high values of aspartate aminotransferase (AST) and alanine aminotransferase (ALT). At that time, skin lesions in this patient were as follows: a multifocal erythematous scaly patchies with plaques involving forearms, thighs, and knees, which were more prominent on the left side. The patient was not a habitual drinker and was on regular medication with acitretin and non-steroidal anti-inflammatory drugs (NSAIDs). With regard to the possibility of toxic hepatitis, several medications, including the acitretin and NSAIDs, were discontinued and hepatotonics were started. After 6 months, a higher elevation of liver enzymes was noted despite the discontinuation of the suspected hepatotoxic medications, acitretin and NSAIDs. (Fig. 1) AST was 219 U/L (normal value 8-38), ALT was 171 U/L (normal 4-44), alkaline phosphatase was 90 U/L (normal 30-130), and gamma glutamyl transferase was 232 U/L (normal 16-70). The patient was negative for viral hepatitis and positive for hepatitis B antibody by serologies, but had new elevations in autoimmune markers, including antinuclear antibody (ANA with a titer of >1:2,560), double-stranded DNA antibody (anti-dsDNA with a titer of 44.0 IU/mL), and quantitative immunoglobulins with an IgG of 5,568 mg/dL (normal 700-1,600). Anti-smooth muscle and anti-liver/kidney microsomal antibodies were negative. Liver ultrasonography (USG) showed mild degree of hepatic steatosis.
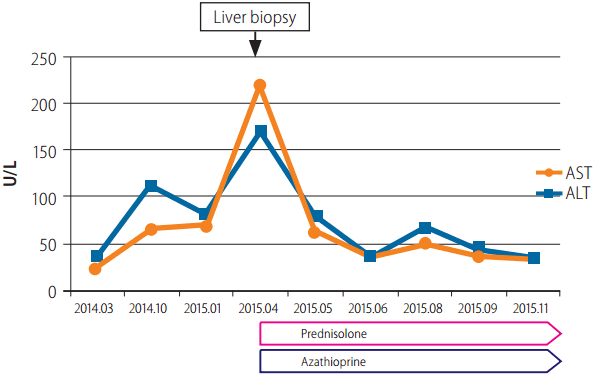
Elevated liver enzymes were noted 6 months after discontinuation of suspected hepatotoxic drugs. Liver biopsy was performed and autoimmune heapatitis (AIH) was diagnosed. Two months of prednisolone and azathioprine normalized the enzymes. AST, aspartate aminotransferase; ALT, alanine aminotransferase.
A liver biopsy was performed to identify the cause of the abnormal liver enzymes. Histological findings showed mild fatty change, diffuse inflammation of the portal tracts with lymphocytes and numerous plasma cells, and moderate interface hepatitis in the periportal regions with plasma cells. (Fig. 2) This finding was consistent with AIH. Due to the combination of the liver biopsy findings, the absence of a viral process, and the positive AIH serologies, the patient was diagnosed with AIH according to the modified diagnostic criteria of the International AIH Group.
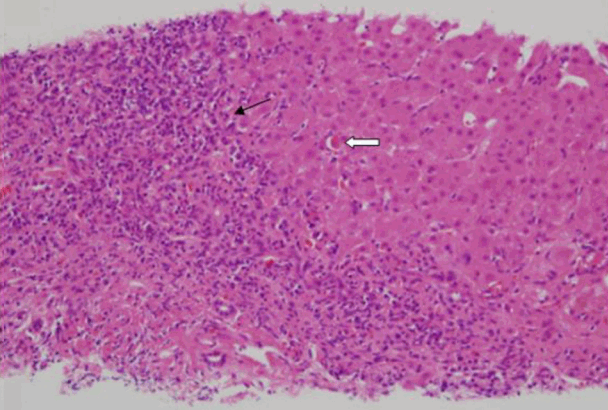
Liver biopsy shows lymphoplasmacytic portal and periportal infiltrates with active interface hepatitis (arrow). An apoptotic liver cell is present (open arrow) (H&E, ×200).
The patient was treated with 30 mg/day of prednisolone with the reduction of the dose 10mg every 2 weeks and 50 mg/day of azathioprine. His liver enzymes improved, then normalized after 2 months of treatment. The serum level of IgG measured after 5 months treatment was 1,802 mg/dL. The patient remains on maintenance therapy of 10 mg/day of prednisolone in combination with 50 mg/day of azathioprine, and no relapse of AIH has been observed.
DISCUSSION
Psoriasis is a chronic, inflammatory, multisystem disorder associated with an escalation of comorbidities leading to significant physical and psychosocial burdens [8]. It is defined by a series of linked cellular changes in the skin, with hyperplasia of epidermal keratinocytes, vascular hyperplasia and ectasia, and infiltration of T-cells [9]. Other autoimmune diseases that can coexist with psoriasis are inflammatory bowel disease, ankylosing spondylitis, and uveitis. A variety of complications can also be associated with the liver. The common risk factors associated with elevated liver enzymes in psoriasis patients are alcoholic hepatitis, viral hepatitis, drug-induced toxic hepatitis, and neutrophilic cholangitis [8]. Several recent studies have found an increased prevalence of non-alcoholic fatty liver disease (NAFLD) in psoriasis patients, indicating that psoriatic inflammation is an independent risk factor for NAFLD [8,10]. In parallel with this result, liver USG also revealed steatosis in our patient. However, this finding is not thought to be correlated with elevated liver enzymes. Drug-induced toxic hepatitis is associated with MTX, acitretin, and anti-TNF-α agents in the management of psoriasis [8]. The elevated liver enzymes were not improved in our patient after the discontinuation of suspected hepatotoxic drugs, with the exclusion of other attributable causes, and he had not been treated with MTX or anti-TNF-α agents. Therefore, we ruled out drug-induced toxic hepatitis, tested autoimmune markers, and performed a liver biopsy to consider the possibility of AIH.
A reliable diagnosis of AIH can be made using the simplified scoring system suggested by the International AIH Group [11]. This revised simplified scoring system allowed the definite diagnosis of AIH in our patient, who had a score of 7 points due to the presence of high IgG levels, ANA seropositivity, and liver histological features compatible with AIH, as well as the absence of viral hepatitis.
AIH is predominantly seen in young women (sex ratio 3.6:1), but is rare, with a mean incidence of 1-2 per 100,000 and a point prevalence of 11-17 per 100,000 [5]. Like other autoimmune diseases, the etiology of AIH is not fully understood, although both genetic and environmental factors are involved in its expression [4]. The treatment of AIH is prednisolone alone or in combination with azathioprine, and most patients with AIH respond well to therapy and have a good prognosis [4]. However, a minority of patients may present with acute liver failure, requiring liver transplantation [4,5]. Additionally, patients with AIH may present with other autoimmune diseases, such as primary biliary cirrhosis and autoimmune thyroiditis [11,12]. According to a study by Culmali et al., three patients with overlap syndrome had concurrent psoriasis [13]. Approximately 9% of AIH cases are triggered by drugs [14]. Several drugs, including minocycline, nitrofurantoin, atorvastatin, and anti-TNF-α agents, have been proposed to induce AIH [5,14]. However, we could rule out drug-induced AIH in our patient because he had not been exposed to these drugs.
With regard to the present case, when psoriasis patients with abruptly elevated liver enzymes do not have a definite cause, such as alcohol consumption, drugs, or viral hepatitis, AIH should be considered.
To date, the association between psoriasis and AIH remains unclear, but it has been reported that the risk of AIH may be increased in patients with psoriasis because this condition and AIH share a similar pathogenesis in which tissue-resident memory T-cells play an important role [15]. It is applicable to our case report that concurrent psoriasis and AIH are not merely coincidental.
In this case, AIH occurred in a patient with psoriasis who did not receive immunosuppressive therapy, such as anti-TNF-α agents or MTX. This confirms that AIH should be carefully considered in the setting of elevated liver enzymes in psoriasis patients who have not undergone immunosuppressive therapy.
Notes
Conflicts of Interest:The authors have no conflicts to disclose.
Abbreviations
AIH
autoimmune hepatitis
ALT
alanine aminotrasferase
ANA
antinuclear antibody
AST
aspartate aminotransferase
ds-DNA
double-stranded DNA
MTX
methotrexate
NAFLD
non-alcoholic fatty liver disease
NSAIDs
non-steroidal anti-inflammatory drugs
TNF
tumor necrosis factor
USG
ultrasonography
