Management of hepatitis C viral infection in chronic kidney disease patients on hemodialysis in the era of direct-acting antivirals
Article information
Abstract
The advent of novel, direct-acting antiviral (DAA) regimens for hepatitis C virus (HCV) infection has revolutionized its treatment by producing a sustained virologic response of more than 95% with few side effects and no comorbidities in the general population. Until recently, ideal DAA regimens have not been available to patients with severe renal impairment and end-stage renal disease because there are limited data on the pharmacokinetics, safety, and efficacy of treatment in this unique population. In a hemodialysis context, identifying patients in need of treatment and preventing HCV transmission may also be a matter of concern. Recently published studies suggest that a combination of paritaprevir/ ritonavir/ombitasvir and dasabuvir, elbasvir/grazoprevir, or glecaprevir/pibrentasvir successfully treats HCV infection in chronic kidney disease stage 4 or 5 patients with or without hemodialysis.
INTRODUCTION
Hepatitis C virus (HCV) infection is one of the main causes of acute and chronic hepatitis, cirrhosis, and hepatocellular carcinoma [1]. In 2014, more than 115 million people were infected with HCV worldwide, which accounts for 1.6% of the world’s population [2]. The prevalence of HCV in hemodialysis patients in Europe and the USA varies from 3 to 20%, which is higher than in the general population [3]. In Korea, 0.78% of adults were seropositive for anti-HCV antibodies in health examinations of 291,314 adults older than 20 years of age from 29 health examination centers [4]. Meanwhile, the prevalence of anti-HCV was 5.9-14.7% in a previous study of more than 200 patients with chronic kidney disease, and 4% in the 2016 Korean Society of Nephrology report [5].
HCV is both a cause and a consequence of renal impairment [3]. HCV infection may induce renal disease (i.e., cryoglobulinemia membrano-proliferative glomerulopathy and non-cryoglobulinemic nephropathy) [6]. HCV infection is highly prevalent among chronic kidney disease (CKD) subjects undergoing hemodialysis than in the general population due to medical procedures, and is mainly related to parenteral exposure [7]. HCV infection has been associated with both liver disease-related deaths and cardiovascular mortality in hemodialysis patients [7]. The vast majority of HCV chronic infections in the hemodialysis setting are currently attributable to nosocomial transmission [7].
Recently, several outbreaks of HCV have occurred in hemodialysis units. While the exact mechanism of HCV transmission could not be ascertained in each facility where an outbreak occurred, several breaches in infection control practices, particularly improper injection-medication practices and suboptimal cleaning and disinfection, were identified. In the course of investigating outbreaks, some of the affected facilities were noted to be non-adherent with established guidelines for screening and managing hemodialysis patients for new HCV infection [8,9]. Since most new HCV infections were asymptomatic, routine screening of hemodialysis patients is crucial for the prompt identification of new infections and outbreaks among these patients [2,3,6]. Reasons for this high prevalence are due to blood transfusions (before effective screening of blood donors for HCV was instituted), nosocomial transmission in dialysis units, and transmission by kidney grafts. HCV-infected dialysis patients have a poor prognosis due to cirrhosis, hepatocellular carcinoma, and cardiovascular disease. Epidemiological studies on the potential risk factors for infection have found that HCV transmission occurs mainly by parenteral exposure to contaminated blood or blood products, or by illegal drug injection.
Until 2011, therapy combining subcutaneous pegylated interferon (PEG-IFN) and oral ribavirin was considered the standard of care for HCV treatment in CKD patients despite a high prevalence of side effects and poor clinical tolerance [7]. New direct-acting antivirals (DAAs) offer dramatically improved efficacy in the general population, but there is only limited information on the pharmacokinetics, safety, efficacy, and dosage of DAAs in the context of hemodialysis [7]. This review will focus on the prevention and therapies available for HCV in CKD patients undergoing hemodialysis.
SCREENING OF HCV INFECTION IN HEMODIALYSIS PATIENTS
According to the recommendations of the Korean Association for the Study of the Liver (KASL), anti-HCV should be tested in CKD patients on hemodialysis for the first time or when they are transferred from other dialysis units [4]. According to the recommendations of the Asian-Pacific Association for the Study of the Liver (APASL), in addition to the serologic tests, RT-PCR should be also performed in these clinical settings [10]. CKD patients on hemodialysis with unexplained abnormal liver-related biochemical tests who are continuously anti-HCV–negative should undergo an HCV RNA assay [4]. The optimal interval for surveillance of HCV infection in anti-HCV negative patients in dialysis units is 6-12 months [4].
PREVENTION OF HCV TRANSMISSION IN HEMODIALYSIS UNITS
HCV is transmitted primarily through percutaneous blood exposure [11]. The number of years spent on dialysis therapy has been identified as an independent risk factor for HCV infection in hemodialysis patients [12,13]. Long-term hemodialysis might increase the cumulative HCV infection risk from exposure in hemodialysis units, as well as other non-hemodialysis healthcare exposures [11]. A recent review summarized 16 outbreaks in nonhospital care settings in the United States that resulted in 275 persons acquiring HCV infection [14]. Six of these outbreaks occurred in outpatient hemodialysis units and resulted in at least 40 HCV infections in dialysis patients [14]. These outbreaks in hemodialysis facilities involved lapses in infection control practice. The most common categories of lapses include: (1) improper parenteral medication handling and precaution, and (2) inadequate environmental cleaning and disinfection between patient treatments [11]. Based on the summarized Unites States investigations from 1998 to 2008, the following medication practices were linked to patient-to-patient HCV transmission in hemodialysis facilities: injections prepared in a contaminated environment, including at the patient treatment station instead of in a separate clean area; use of mobile medication carts to deliver parenteral medications to patients; and use of single-dose medication vials to provide medication for more than one patient [14,15]. Poor environmental cleaning and disinfection practices also have been identified during investigations of causes of HCV transmission. Indeed, HCV RNA has been detected on external surfaces of dialysis machines, a dialysate connector, and a shared waste cart [11,16]. HCV persists in an infectious state at ambient room temperature in the environment for at least 16 hours [17,18]. The frequency of blood contamination in this setting and the environmental stability of HCV highlights the potential for direct or indirect transmission from contaminated surfaces or objects [11]. In 2001, the Centers for Disease Control and Prevention published guidelines to prevent the transmission of HCV and other infections among maintenance hemodialysis patients [19]. The recommended precautions for infection control in hemodialysis units included the following: all single-use injectable medication vials should be dedicated for single use in a single patient; hand hygiene should be performed frequently during routine patient care; disposable gloves should be worn when caring for patients or touching their patient’s equipment at the dialysis station; gloves should be removed and hands should be washed between each patient or station; items brought into the dialysis station should be either disposed of or cleaned and disinfected before being taken to a common clean area or used for another patient; the dialysis station, including the chairs, tables, and machines, should be cleaned and disinfected between patients; clean areas should be clearly designated for the preparation, handling, and storage of medications and unused supplies and equipment; clean areas should be clearly separated from contaminated areas where used supplies and equipment are handled; external venous and arterial pressure transducer filters/protectors should be used for each patient during treatment to prevent the contamination of the pressure monitors of dialysis machine; and cover all dialyzer ports for all reprocessed dialyzers and place all used dialyzers and tubing in leak-proof containers for transport from station to the reprocessing or disposal area [19].
CLINICAL COURSE OF HCV INFECTION IN CKD PATIENTS
Acute hepatitis C
In the general population, most acute infections are asymptomatic and anicteric [9]. Typically, 10–14 weeks after infection, an increase in the serum alanine aminotransferase (ALT) level occurs [8]. The early peak in HCV viral RNA load is sometimes followed by a transient decline, and approximately 15–20% of patients will clear acute infection [9]. Early treatment is more effective than delayed treatment [20]. The optimal treatment regimen for acute HCV infection with PEG-IFN has not been established, but 12 weeks of subcutaneous PEG-IFN monotherapy is recommended [4]. The proportion of patients who have a sustained virologic response (SVR) ranges from 65% to more than 85% [20]. Optimal treatment regimen for DAAs has not yet been defined in this clinical setting [21].
Like in the general population, acute infections are usually asymptomatic and anicteric in hemodialysis patients [7]. Viral clearance is uncommon in hemodialysis patients, and occurs in less than 5% of patients. Therefore, acute infections should be treated as soon as the diagnosis is established, whenever possible [22,23].
Chronic hepatitis C
Most individuals newly infected with HCV eventually develop chronic infection (75%-85%) and chronic liver disease (60%-70%) [11]. Long-term sequelae of chronic HCV infection include cirrhosis and hepatocellular carcinoma [11]. Chronic HCV infection is also an important cause of morbidity and mortality in hemodialysis patients and has been associated with both liver disease-related deaths (due to complications of cirrhosis and hepatocellular carcinoma) and cardiovascular mortality [24-26].
TREATMENT OF HCV INFECTION IN PATIENTS WITH CHRONIC KIDNEY DISEASE STAGE 4-5 INCLUDING HEMODIALYSIS PATIENTS
Conventional treatment using pegylated interferon and ribavirin
Until 2011, the standard of care was a combination of PEG-IFN and oral ribavirin [21]. The goal of this combination treatment was to develop an SVR, that would be, in effect, a cure. SVR are observed in only approximately 35% of dialysis patient [27]. Furthermore, this regimen is associated with significant adverse events, and is poorly tolerated in patients with advanced disease including CKD patients [21,28].
Data for hemodialysis patients with acute HCV infection are scarce, with small sample sizes [7]. In addition, most studies report results using standard interferon [7]. Only two studies have reported data of PEG-IFN therapy in hemodialysis patients [7,29,30]. In these studies, the SVR rate was 59%, with 9% of the patients dropping out of the study [7]. As a result of these studies, it is recommended that these types of patients are treated for acute HCV infection with PEG-IFN monotherapy, regardless of genotype [7].
In hemodialysis patients with chronic HCV infection, there have been several trials of treatment, but are mostly uncontrolled and use different therapeutic regimens [7]. Overall SVR rates derived from meta-analysis appear not to be different from that of patients treated with standard interferon or PEG-IFN (i.e., they range from 33% to 60%) [7]. Ribavirin is primarily renally cleared, mainly situated in the erythrocyte and not effectively cleared from the body during hemodialysis [3]. The addition of ribavirin seems to provide a significant increase in SVR, but those patients with renal impairment or who are dependent on hemodialysis often tolerate ribavirin poorly, even after dose adjustments [3,7].
Recent studies on new DAAs regimens
Over the previous 10 years, advances in HCV cell cultures have improved our understanding of HCV virology, which has led to the development of many new DAAs that target key components of HCV replication [21]. Furthermore, new DAAs allow for simplified and shortened treatments for HCV that can be given as oral regimens with increased tolerability and efficacy compared to conventional treatment with PEG-IFN and ribavirin [21].
Most DAAs are hepatically cleared. Among the currently approved DAAs, only sofosbuvir is primarily renally cleared [31]. In general, renal impairment results in increased drug concentrations of renally cleared drugs [3]. There are limited data on the pharmacokinetics, safety, efficacy, and dosage in these special populations [3].
In 2013, the approval of the pan-genotypic NS5B inhibitor sofosbuvir revolutionized the treatment of HCV infection in the general population by leading to high rates of SVR with few side effects [32]. However, the use of sofosbuvir is restricted to CKD patients with an estimated GFR (eGFR) of at least 30 mL/min because it has not been studied in patients with an eGFR below 30 mL/min. The active metabolite of sofosbuvir, GS331007, is eliminated by the kidney, and levels of sofosbuvir and GS331007 are substantially higher in patients with severe renal impairment (eGFR <30 mL/min) or end-stage renal disease (ESRD) on hemodialysis [33].
Currently, there is no definitive treatment guideline for patients with CKD on hemodialysis (Table 1) [10,34-36]. Recently, several studies on the efficacy and safety of DAAs for patients with stage 4 or 5 CKD have been reported (Table 2) [37-43]. In recent studies, available anti-HCV regimens using DAAs for patients with stage 4 or 5 CKD could be classified into two groups: sofosbuvir-containing regimens and sofosbuvir-excluding regimens. Saxena et al. reported the result of full dose sofosbuvir-containing regimens in HCV-infected patients with renal impairment (eGFR ≤45 mL/mi/1.73 m2) [37]. They suggested that SVR was achieved in 88% of patients with severe renal impairment (eGFR <30mL/min/1.73 m2) who were treated with full dose sofosbuvir-containing regimens. However, these patients showed worsening renal dysfunction and serious adverse events regardless of use of ribavirin [37]. Among those CKD patients, 5 patients were treated with hemodialysis (HD) and achieved a SVR at 12 weeks after treatment ended (SVR12). SVR rates did not differ among CKD stage 4-5 patients, regardless of their hemodialysis status. Furthermore, studies involving sofosbuvir-containing regimens in HCV-infected patients with stage 4 or 5 CKD enrolled small numbers of patients and experienced limitations in applying these regimens in a real clinical setting.
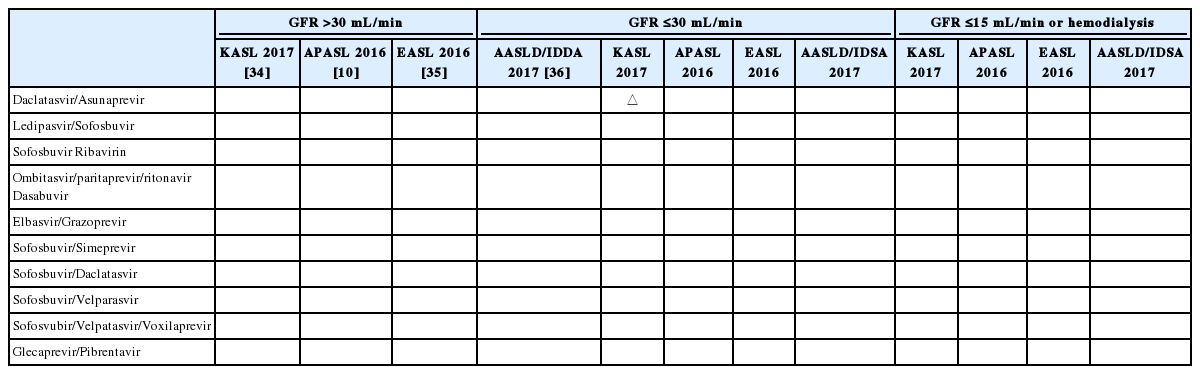
Comparison of the recommendations of the AASLD, EASL, APASL and KASL for treatment of chronic HCV infection using DAAs
There are four available sofosbuvir-excluding regimens that are safe and efficacious in HCV-infected patients with stage 4 or 5 CKD. Pockros et al. reported the results of a study of the efficacy of paritaprevir/ritonavir/ombitasvir/dasabuvir combination therapy for genotype 1 HCV-infected patients with stage 4 or 5 CKD [40]. The majority of patients had stage 5 CKD with 14 patients on hemodialysis. Notably, a SVR was achieved in 90% of CKD stage 4 or 5 patients, whereas 93% of the 14 patients treated with HD achieved a SVR12. Suda et al. studied the efficacy and safety of daclatasvir and asunaprevir combination therapy for genotype 1 HCV-infected patients with chronic hemodialysis patients [41]. They found that this regimen for hemodialysis patients was highly effective and welltolerated. Furthermore, the SVR12 was 95.5%. One patient discontinued treatment at week 12 due to ALT elevation and achieved a SVR12. Roth et al. reported the results of a phase 3 clinical trial, which was the largest trial to date in a cohort of 235 patients with HCV infection in stage 4-5 chronic disease patients. In that trial, patients with chronic genotype 1 HCV infection were treated with an oral, once-daily grazoprevir and elbasvir combination therapy for 12 weeks, which results in a SVR12 of 99% [42]. Among CKD patients, 179 were hemodialysis-dependent, of whom 99% achieved a SVR12. Moreover, SVR rates did not differ among CKD stage 4-5 patients, regardless of hemodialysis use. One recently published study suggested that treatment with glecaprevir and pibrentasvir for 12 weeks produced a SVR12 of 98% in patients with stage 4 or 5 CKD irrespective of HCV genotypes [43]. In total, 82% of those patients had undergone hemodialysis at baseline, of whom 99% achieved a SVR12.
CONCLUSION
Novel DAAs have brightened the future of hemodialysis patients with HCV infections as they represent an avenue of a potential cure from HCV infection. This goal can be achieved by combining prevention and cure, rather than by relying only on a cure. Therefore, studies that identify ideal DAAs regimens to treat HCV infection in hemodialysis patients should be conducted along with improvements in the practice of standard precautions that prevent nosocomial HCV infection. By combining these two approaches, it is possible to eradicate HCV from hemodialysis units. According to recent studies, the most recommended DAA regimens in patients with HCV genotype 1-infected stage 4 or 5 CKD with or without hemodialysis are elbasvir/grazoprevir or a combination of paritaprevir/ritonavir/ombitasvir with dasabuvir, for which there is no need for dose modification. In the near future, glecaprevir/pibrentasvir combination therapy will be an important treatment modality for patients with stage 4 or 5 CKD with or without hemodialysis and HC V infection, regardless of genotype.
Notes
Author's contribution
Ko SY and Choe WH equally contributed to this paper with conception and design of the study, literature review and analysis, drafting and critical revision and editing, and final approval of the final version.
Conflict of Interest
The authors have no conflicts to disclose.
Abbreviations
ALT
alanine aminotrasferase
APASL
Asian-Pacific Association for the Study of the Liver
CKD
chronic kidney disease
DAAs
direct-acting antivirals
ESRD
endstage renal disease
eGFR
estimated glomerular filtration rate
HCV
hepatitis C virus
KASL
Korean Association for the Study of the Liver
PEG-IFN
pegylated interferon
SVR
sustained virologic response

