Impact of nationwide hepatocellular carcinoma surveillance on the prognosis in patients with chronic liver disease
Article information
Abstract
Background/Aims
This study aimed to investigate the effect of hepatocellular carcinoma (HCC) surveillance using the Korea National Liver Cancer Screening Program on the receipt of curative treatment for HCC and mortality in patients with chronic liver disease.
Methods
This population-based cohort study from the Korean National Health Insurance Service included 2003 to 2015 claims data collected from 1,209,825 patients aged ≥40 years with chronic hepatitis B, chronic hepatitis C, and liver cirrhosis. Patients were divided according to HCC surveillance using ultrasonography and serum alpha-fetoprotein every 6–12 months. The study outcomes were the receipt of curative treatment (surgical resection, radiofrequency ablation, or liver transplantation) and all-cause mortality.
Results
The study population consisted of 1,209,825 patients with chronic hepatitis B, chronic hepatitis C, and liver cirrhosis (median age, 52.0 years; interquartile range, 46–55 years; 683,902 men [56.5%]). The proportion of participants who underwent HCC surveillance was 52.7% (n=657,889). During 10,522,940 person-years of follow-up, 74,433 HCC cases developed, including 36,006 patients who underwent curative treatment. The surveillance group had a significantly higher proportion of curative treatment for HCC than the non-surveillance group after adjusting for confounding factors (adjusted hazard ratio [HR], 5.64; 95% confidence interval [CI], 5.48–5.81). The surveillance group had a significantly lower mortality rate than the non-surveillance group (adjusted HR, 0.56; 95% CI, 0.55–0.56).
Conclusions
HCC surveillance using the national screening program in patients with chronic viral hepatitis or liver cirrhosis provides better opportunity for curative treatment for HCC and improves overall survival.
Graphical Abstract
INTRODUCTION
Hepatocellular carcinoma (HCC) accounts for 75–85% of all primary liver cancers and is the fourth most common cause of cancer related death worldwide [1]. Although overall survival in patients with HCC has improved, the mortality rate is still high [2]. To reduce the mortality rate, early detection of HCC is emphasized to increase the opportunity for curative treatment. Most HCCs develop in the background of chronic liver disease. In particular, the risk of HCC is higher in patients with chronic viral hepatitis (hepatitis B virus [HBV] infection or hepatitis C virus [HCV] infection), or cirrhosis of any cause [3].
A meta-analysis revealed that HCC surveillance was beneficial in detecting early stage tumors, increasing the chance of curative therapy, and improving overall survival in cirrhotic patients [4]. Most guidelines recommend HCC surveillance in high risk groups (cirrhosis of any cause or chronic hepatitis B [CHB]) using ultrasonography and/or serum alpha-fetoprotein (AFP) every 6 months [3-5]. However, there is a lack of existing clinical evidence on the effect of HCC surveillance on chronic liver disease prognosis, and there are only two randomized clinical trials on HCC surveillance in Chinese patients with CHB [6-8]. Besides, one of those randomized trials used serum AFP only for HCC surveillance and did not show a reduction in mortality in patients who underwent surveillance [7,9]. In addition, the adherence to HCC surveillance is poor even in high risk groups [10].
The highest incidences of HCC are recorded in East Asia and Sub-Saharan Africa [1]. In those areas, HCC surveillance is particularly crucial for reducing the disease burden and improving the prognosis of patients with chronic liver disease. In South Korea, HCC is the 5th most common cancer and 2nd highest cause of cancer death [9]. The National Liver Cancer Screening Program (NLCSP) for HCC surveillance has been conducted in South Korea since 2003 [11]. This study aimed to investigate the impact of nationwide surveillance on the receipt of curative treatment for HCC and the mortality of chronic liver disease in an area with a high incidence of HCC. This nationwide population-based study included Korean patients aged ≥40 years with CHB, chronic hepatitis C (CHC), and liver cirrhosis in South Korea.
MATERIALS AND METHODS
Study design and population
This cohort study used claims data from the Korean National Health Insurance Service (NHIS) database from 2002 to 2017 [12]. The NHIS is the sole public payer for Korea’s mandatory universal medical insurance system. All clinics and hospitals in Korea submit data to the NHIS for inpatient hospitalizations and outpatient visits to claim reimbursements for patient care. The NHIS database comprises four databases on insurance eligibility, medical treatments, medical care institutions, and general health exams, and the general health exams database included the NLCSP data [13]. The Korean government has been running the national cancer screening program for the whole population since 1999 [11]. The program was firstly introduced for gastric cancer, breast cancer, and cervical cancer in 1999, and thereafter, the screening program for liver cancer was conducted in 2003. Colon cancer screening was introduced in 2004. From 2003 onwards, the NLCSP in Korea began to provide ultrasonography and serum AFP for HCC surveillance of patients aged ≥40 years with CHB, CHC, or liver cirrhosis [14]. Repeat screening for HCC surveillance was recommended every 6 months from 2003–2010, every 12 months from 2011–2015, and every 6 months since 2016.
The inclusion criteria for this study were patients who were 40 years of age or older and who were newly diagnosed with CHB, CHC, or liver cirrhosis between January 1, 2003 and December 31, 2015 (n=1,376,509). CHB, CHC, and liver cirrhosis were defined based on the International Classification of Diseases, tenth revision (ICD-10) codes: CHB (B18.0, B18.1, and Z22.5), CHC (B18.2), liver cirrhosis (K70.2, K70.3 K74, K74.1, K74.2, K74.3, K74.4, K74.5, K74.6, K76.5, and K76.6). We excluded patients who had any cancer in 2002 (n=41,349), those who were newly diagnosed with cancer between 2003 and the initial diagnosis of liver disease (n=102,857), those diagnosed with HCC within three months of a liver disease diagnosis (n=47,660), and those who died within 6 months of a liver disease diagnosis (n=46,940). The final sample size was 1,209,825 (683,902 men and 525,923 women; Fig. 1). The Institutional Review Board (IRB) of Samsung Medical Center approved this study and waived the requirement for informed consent because we used publicly available de-identified data (IRB No.: SMC 2018-03-019).
Measurements
HCC was defined as the presence of the same C code (ICD-10 code C22.0) more than three times within a year, or inpatient hospitalization with a C22.0 code. The C codes are carefully reviewed by the NHIS because they have implications for additional benefits for patients. Once a person has a C code, it is carried forward in the medical records and claims are created for that patient. Therefore, cancer diagnoses based on claims are considered reliable. We excluded patients with any history of cancer using a 1-year look-back window; therefore, patients with a prior diagnosis of cancer (C code), excluding those with a prior diagnosis at any time (had a history of cancer), and those diagnosed with cancer in the previous year were excluded. In this study, curative treatment for HCC was defined as surgical resection, radiofrequency ablation (RFA), or liver transplantation as the initial therapy [15].
Information on HCC surveillance was based on the results of the NLCSP, and patients who had undergone at least one screening were considered to be patients with HCC surveillance. When we evaluated the effect of HCC surveillance, the effect continued until 6 months after surveillance. Potential confounders included age, sex, year of diagnosis of chronic liver disease, type of liver disease, comorbidities, residential area and income percentile. Co-morbidities during the year prior to the screening exam were defined using ICD-10 codes and were summarized using the Charlson comorbidity index (CCI) [16]. In addition, the use of antiviral agents was evaluated using the dataset on the prescription drugs. We searched for the drug codes of antiviral agents for HBV (lamivudine, adefovir, clevudine, telbivudine, entecavir, tenofovir, and peg-interferon) and HCV (peg-interferon, ribavirin, daclatasvir, asunaprevir, sofosbuvir, and ledipasvir/sofobuvir). Finally, vital status through December 31, 2017 was ascertained from mortality and population registration data from Statistics Korea. Among all cause-death, the liver related mortality was defined as presence of admission with liver cancer or liver disease within a month before death.
Statistical analysis
To determine the proportion of patients who underwent HCC surveillance, we calculated the denominator as the cumulative number of high-risk groups that did not register incident HCC or death during the year. The primary outcome of this study was the receipt of curative treatment for HCC and the secondary outcomes were HCC incidence, liver-related mortality, and all-cause mortality. Participants were included in the study at the baseline clinic visit and were followed-up until HCC development, death, or the end of the study period (December 31, 2017). For the mortality outcomes, participants were followed up until death or the end of the study period. The study exposure was HCC surveillance, which is considered a time-varying variable to control for immortal time bias. For each HCC surveillance conducted, participants who were surveyed contributed person-time to the exposed group starting after the date of the initial surveillance until 6 months after surveillance. Since the exposure was treated as a time varying covariate, if a patient stopped midway for a few years and then resumed every 6 months, the patient was re-considered as part of the surveillance group from the time since their surveillance was resumed. Basically, in a time-dependent analysis, the follow-up time for each patient is divided into different time windows. First, for each time window, a separate Cox analysis is performed using the specific value of the time-varying variable at the beginning of that specific time window. Second, a weighted average of all the time window-specific results is calculated [17]. We compared the risk of patients who underwent the HCC surveillance test versus those who did not using Cox proportional hazards regression models to estimate hazard ratios (HRs) with 95% confidence intervals (CIs) for incident HCC in all patients and for all-cause mortality and liver-related mortality. We adjusted for age, sex, year of liver disease diagnosis, region, income percentile, type of liver disease (HBV, HCV, or liver cirrhosis), CCI score, and the use of antiviral agents. We examined the proportional hazard assumption using plots of the log(-log) survival function and Schoenfeld residuals.
This study also analyzed the impact of surveillance in patients with HCC. We investigated differences in mortality according to surveillance in patients with HCC. Furthermore, we performed a sensitivity analysis to control for lead-time bias, which represents improved survival due to earlier diagnosis. The expected additional follow-up duration due to the lead-time was calculated and subtracted from the observed survival time. The HCC sojourn time was assumed to be 70 or 140 days, according to estimations reported in previous studies [18]. All analyses were performed using STATA version 14 (StataCorp LP, College Station, TX, USA) and SAS 9.4 (SAS Institute, Cary, NC, USA).
RESULTS
Clinical characteristics of the enrolled patients
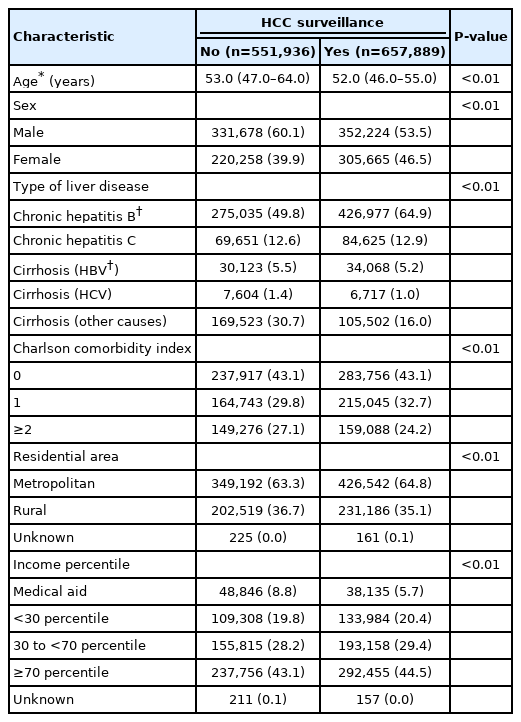
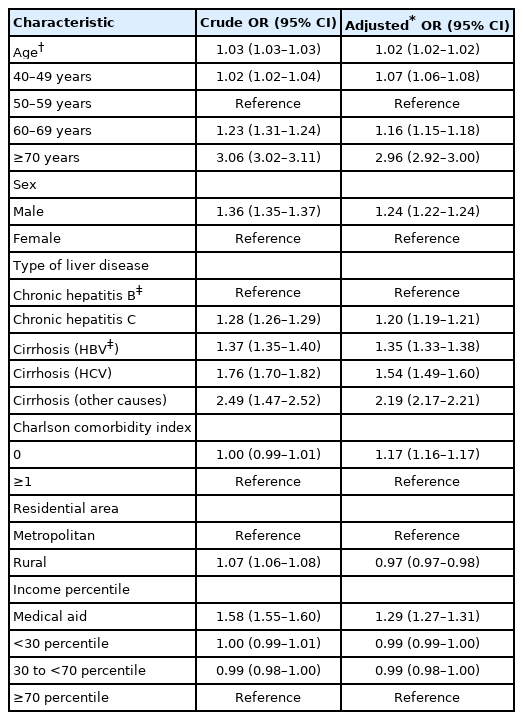
The proportion of participants who underwent HCC surveillance was 52.7% (657,889/1,209,825) during the entire study period. The proportion of participants increased progressively each year, from 0.1% in 2003 to 21.6% in 2017 (Supplementary Fig. 1). The median (interquartile range) age at the time of diagnosis of chronic liver disease in the surveillance group was 52 years (46–55), and 53.6% of the patients were men. The surveillance group was younger, more likely to be female, and more likely to have CHB than the non-surveillance group. The non-surveillance group was more likely to live in rural areas and receive medical aid (Table 1). We investigated the factors associated with non-participation in HCC surveillance. In multivariable analysis, participants who were aged 60–69 years (odds ratio [OR], 1.16; 95% CI, 1.15–1.18) or ≥70 years (OR, 2.96; 95% CI, 2.92–3.00), were male (OR, 1.24; 95% CI, 1.22–1.24), had no comorbidities (OR, 1.17; 95% CI, 1.16–1.17), had CHC (OR, 1.20; 95% CI, 1.19–1.21) or cirrhosis, and were medical aid beneficiaries (OR, 1.29; 95% CI, 1.27–1.31) were significantly associated with an increased probability of nonparticipation in HCC surveillance (Table 2).
Detection of HCC and receipt of curative treatment for HCC by surveillance
During 10,522,940 person-years of follow-up, 74,433 HCC cases were observed. The HCC incidence rates per 1,000 person years were 6 and 23 in the non-surveillance (n=551,936) and surveillance (n=657,889) groups, respectively. The surveillance group had a significantly higher detection rate of HCC than the non-surveillance group after adjusting for age at diagnosis of the liver disease, sex, type of the liver disease, year of chronic liver disease diagnosis, CCI score, residential area, and income percentile (adjusted HR, 5.34; 95% CI, 5.23–5.46). Similarly, the proportions of patients receiving curative treatment for HCC were 3 and 12 per 1,000 person-years in the non-surveillance and surveillance groups, respectively, and the surveillance group was more likely to have the opportunity of curative treatment for HCC than did the non-surveillance group (adjusted HR, 5.64; 95% CI, 5.48–5.81) (Table 3). The surveillance group had a significantly higher rate of patients receiving curative treatment for HCC than did the non-surveillance group regardless of cirrhosis (adjusted HR, 6.41; 95% CI, 6.18–6.65 in no cirrhosis; adjusted HR, 4.64; 95% CI, 4.42–4.87 in cirrhosis) (Table 3). The positive association between HCC surveillance and receipt of curative treatment for HCC was consistent in most pre-specified subgroups analyzed (Fig. 2A). In the subgroup analysis, there was a prominent effect of national screening on the receipt of curative treatment for HCC in the following patients: those in their 40s, males, those with CHB and those with no comorbidities.

Detection of HCC and receipt of curative treatment for HCC in chronic liver disease by HCC surveillance (n=1,209,825)
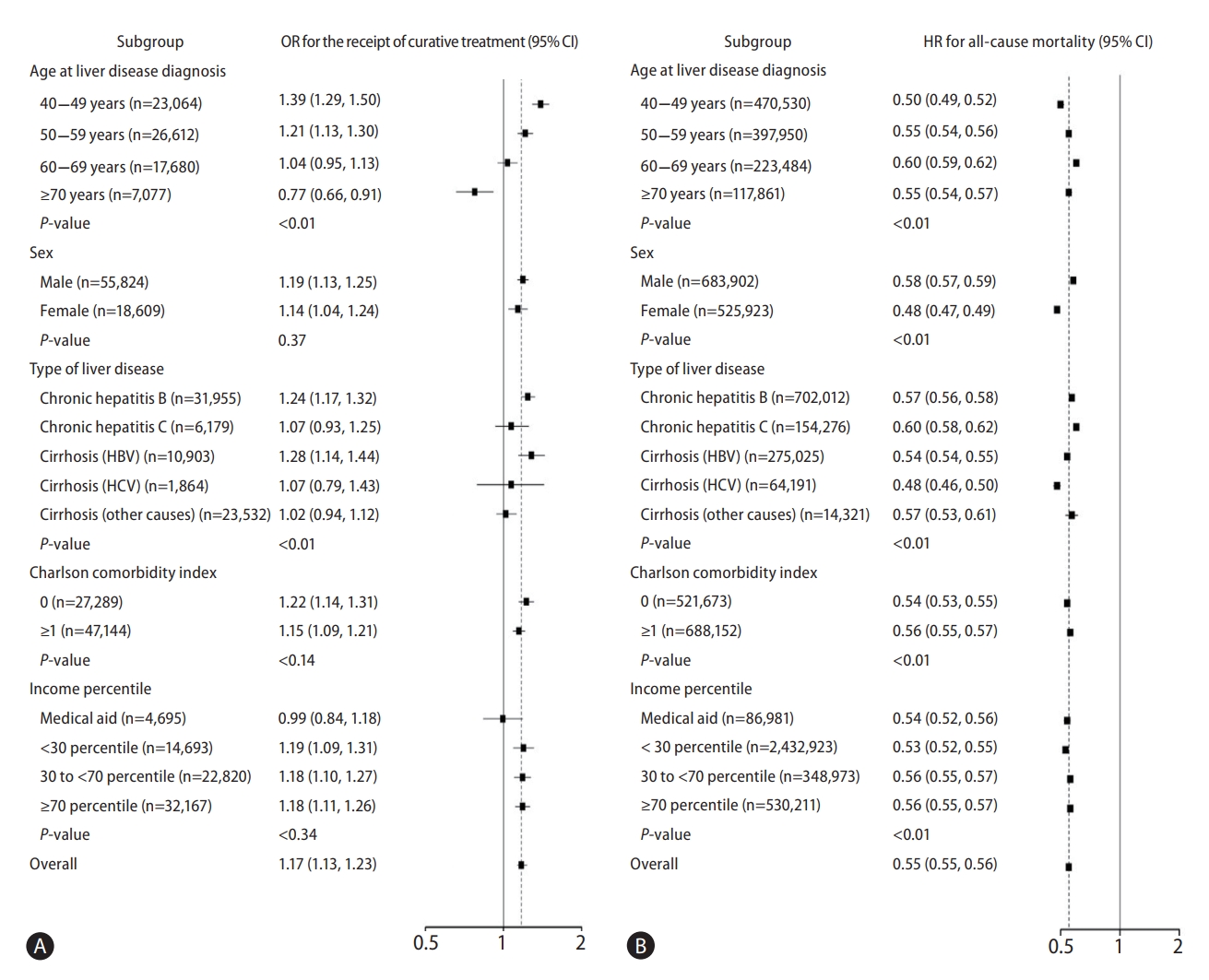

Subgroup analysis for the receipt of curative treatment for hepatocellular carcinoma (A) and all-cause mortality (B) in patients with hepatocellular carcinoma. Adjusted for age, sex, year of chronic liver disease diagnosis, region, income, hepatitis B virus infection, hepatitis C virus infection, liver cirrhosis, Charlson comorbidity index, and initial treatment modality for hepatocellular carcinoma. OR, odds ratio; HCC, hepatocellular carcinoma; CI, confidence interval; HBV, hepatitis B virus; HCV, hepatitis C virus.
Impact of HCC surveillance on mortality
The impact of HCC surveillance on mortality in patients with chronic liver disease was investigated (n=1,209,825). The all-cause mortality rates were 22 and 12 deaths per 1,000 person-years in the non-surveillance and surveillance groups, respectively, in all participants. Patients who received surveillance had a significantly lower all-cause mortality rate than those who did not (adjusted HR, 0.56; 95% CI, 0.55–0.56) (Table 4). All-cause mortality was significantly lower in the surveillance group than in the non-surveillance group regardless of cirrhosis (adjusted HR, 0.58; 95% CI, 0.57–0.59 in no cirrhosis; adjusted HR, 0.54; 95% CI, 0.53–0.55 in cirrhosis) (Table 4). Among the patients who died, 143,112 (72%) died because of liver-related causes. The liver-related mortality was also significantly lower in the surveillance group than in the non-surveillance group (adjusted HR, 0.55; 95% CI, 0.54–0.55) regardless of cirrhosis: adjusted HR, 0.63; 95% CI, 0.61–0.64 in no cirrhosis; adjusted HR, 0.54; 95% CI, 0.54–0.55 in cirrhosis (Supplementary Table 1). The impact of HCC surveillance on all-cause mortality reduction was consistent in most of the pre-specified subgroups analyzed (Fig. 2B). In subgroup analysis, there was a prominent effect of national screening on the reduction of mortality in patients: in their 40s, and women.
In addition, we analyzed the impact of surveillance on allcause mortality in patients with HCC (n=74,433) (Supplementary Table 2). The mortality rates per 1,000 person years were 166 and 133 in the non-surveillance (n=47,651) and surveillance (n=26,782) groups, respectively. Among patients with HCC, those who underwent surveillance had a significantly lower mortality rate than those who did not (adjusted HR, 0.81; 95% CI, 0.80–0.83) When we analyzed the impact of time between the surveillance and HCC diagnosis on mortality in the surveillance group, patients who underwent screening within 6 months of receiving the HCC diagnosis (n=26,782), had a significantly lower mortality rate than those who underwent screening at greater than 6 months from screening to diagnosis (adjusted HR, 0.85; 95% CI, 0.82–0.89). Moreover, the mortality was significantly lower in the surveillance group than in non-surveillance group after adjusting for lead-time (70 days): adjusted HR 0.76 with 95% CI, 0.74–0.78 (Supplementary Table 3). The impact of HCC surveillance on mortality reduction was consistent in most prespecified subgroups analyzed in patients with HCC (Supplementary Fig. 2).
DISCUSSION
The present study analyzed national health claim data to evaluate whether HCC surveillance is effective at the receipt of curative treatment for HCC, and is associated with reductions in mortality among patients with CHB, CHC, or liver cirrhosis. Patients who underwent HCC surveillance by ultrasonography and serum AFP were more likely to receive curative treatment for HCC than who did not. HCC surveillance was also beneficial in improving the overall survival and liver-related mortality in these high-risk groups. These findings were consistent with the adjustment for age, sex, etiology of liver disease, presence of cirrhosis, comorbidity, region, income status, year of diagnosis, and the use of antiviral agents for CHB or CHC. Old age, male sex, more comorbidities, presence of CHC or cirrhosis, living in rural areas and being a medical aid beneficiary were associated with non-participation in HCC surveillance.
It is important to detect cancer at an early-stage as it increases the chances of receiving curative treatment and survival. HCC is often asymptomatic and consequently, patients are unaware of the presence of a tumor until HCC has reached an advanced stage [19]. Therefore, the screening test is a crucial strategy for detecting early-stage HCC in patients with chronic liver disease [20]. HCC surveillance is recommended in specific risk groups in terms of threshold HCC incidence for surveillance efficacy with life years gained [3-5]. The guidelines define high-risk groups for HCC surveillance as all cirrhotic patients from any etiology or Asian patients with HBV infection without cirrhosis over 40 years of age. According to these guidelines, all patients with cirrhosis and high-risk hepatitis B patients are at risk for HCC and should undergo surveillance with semiannual ultrasonography and/or serum AFP, which are suggested for the secondary prevention of HCC [3-5]. In our study, we also found that curative treatment for HCC was more likely to be performed among patients in the surveillance group than among those in the non-surveillance group. However, the screening rate was relatively low, even though it is free. In our study, the proportion of patients who participated in the NLCSP at least once during their lifetime was 52.9%. The participation rate was significantly lower in old age, in men, in those with more comorbidities, in those living in rural areas, and in medical aid beneficiaries. Therefore, it is necessary to increase the participation rate of HCC surveillance among these vulnerable patients.
In our study, patients who underwent HCC surveillance had significantly lower mortality rates than those with did not. HCC surveillance which is a part of the national cancer screening program in Korea not only reduced the mortality of HCC but was also instrumental in detecting early-stage HCC among patients with CHB, CHC, and liver cirrhosis. Similar to Korea, the Japanese government has provided HCC surveillance using ultrasonography and serum AFP since the 1980s to people with chronic viral hepatitis, and des-gamma carboxyprothrombin and AFP-L3 fraction tests (serum biomarkers for HCC) have been added to the HCC surveillance program since the 1990s. In Japan, the 5-year survival rate of HCC patients has significantly increased from 25% in the 1980s to 43% in the 2000s [21]. While increased survival rate is also likely due to a number of other factors including advances in the treatment and early detection of HCC, surveillance helped diagnose HCC at earlier stages resulting in increased overall survival [22]. However, in the Japanese studies, there were no comparison groups and they were not able to compare the effectiveness of the screening between the surveillance group and the non-surveillance group. A Taiwanese nationwide cohort study investigated 52,823 patients with HCC and found a significant association between the ultrasonography screening interval and lower mortality. Shorter intervals between screenings were associated with a reduction in mortality in patients with HCC in a time-dependent manner [23]. Similar to the Japanese study, the Taiwanese study only included patients who developed HCC and was not able to evaluate whether HCC surveillance increased the detection of HCC. However, there was a difference in the study designs and study groups between the present study and earlier studies. While the Japanese and Taiwanese studies assessed the impact of HCC surveillance in HCC patients, this study evaluated the outcome of HCC surveillance in groups at high risk for HCC development (CHB, CHC, and liver cirrhosis).
This study had several limitations. First, because we used information from national cancer screening data, this study did not include HCC surveillance performed by private health care providers. This study also did not include information on computed tomography (CT) or magnetic resonance imaging (MRI) which could be used for further evaluation when patients had suspicious dysplastic nodules or indeterminate nodules on ultrasonography. We could not assess the effectiveness of CT and MRI for cancer detection and mortality in terms of HCC surveillance. This may be an unmeasured confounder of study outcomes. Second, this study could not examine the exact tumor stage of HCC because the Korean NHIS does not provide this information (e.g., tumor size, tumor number, distant metastasis). Therefore, this study was determined the receipt of the curative treatment for HCC as the primary outcome instead of the detection of early-stage HCC. The ultimate goal of HCC surveillance in chronic liver disease is the improvement of liver-related mortality including liver cancer mortality. To achieve this goal, HCC surveillance can play a role of the detection of early-stage cancer and this can be linked to curative treatments such as surgical resection, ablation therapy, and liver transplantation. Therefore, most guidelines indicated the primary goal of HCC surveillance was the detection of early-stage HCC and the secondary goals were the receipt of curative treatments, liverrelated mortality, and all-cause mortality [3-5]. It would be the best to determine the detection of early-stage HCC as the primary outcome. However, we inevitably determined the receipt of curative treatments as the primary outcome. Although this study showed that HCC surveillance could provide the opportunity for curative treatment of HCC in chronic liver disease, the treatment modalities did not completely correspond to early-stage tumors in real practice. However, previous studies indicated that there was a similar tendency in the impact of HCC surveillance on the detection of earlystage HCC and the receipt of curative treatment [24,25]. Third, the study did not include data on alcohol and smoking which could influence the development of HCC and mortality in patients with chronic liver disease because the Korean national claim data did not provide information about alcohol intake and cigarette smoking. Another potential limitation is that surveillance may have physical, financial, and psychological harms [26,27]. Finally, in the present study, we evaluated the efficacy of HCC surveillance in CHC patients aged ≥40 years. Most guidelines did not recommend HCC surveillance in CHC patients without cirrhosis because that group did not have a high rate of HCC development satisfying cost-effectiveness of HCC surveillance [3,4]. However, the National Liver Cancer Screening Program in Korea has funded the provision of ultrasonography and serum AFP for HCC surveillance in CHC patients aged 40 years and over regardless of cirrhosis. The findings of the study showed that HCC surveillance is effective in reducing liver-related mortality and improving overall survival in CHC patients without cirrhosis. However, the present study did not assess the cost-effectiveness of HCC surveillance for those patients. Additionally, this study could not exactly evaluate the impact of HCC surveillance in CHC patients who achieved sustained virological response after direct-acting antivirals because direct-acting antivirals in Korea were introduced in August 2015. Therefore, further studies are needed to elucidate the cost-effectiveness and risk stratification of HCC surveillance in patients with CHC. Despite these limitations, this study had several strengths. The present study is representative because it included the entire population aged 40 years and older with CHB, CHC, and liver cirrhosis in South Korea. The NHIS system controls and provides all health services for the whole nation because it is mandatory to join the NHIS system for claim reimbursements in Korea [11]. In addition, the cohort contains extensive information on healthcare usage regarding inpatient and outpatient visits to healthcare institutions and medication histories. Furthermore, this cohort contained the date and the cause of death, which were determined using the national database for cause of death produced by Statistics Korea. Statistics Korea annually reports the cause of death statistics, and a previous study reported the accuracy of the cause of death to be 92% [28]. Thus, this nationwide population-based study was conducted using data from a representative sample of a large number of enrolled patients in an area where HCC incidence rates are high. Furthermore, this study had a long follow-up period (up to 14 years) to evaluate the study outcomes. Therefore, this study has several strengths in terms of representativeness, sample size, and follow-up duration. In conclusion, HCC surveillance using ultrasonography and serum AFP in patients with chronic viral hepatitis or liver cirrhosis provides better outcomes in terms of the receipt of curative treatment for HCC, liver-related mortality, and overall survival. The results of this study provide concrete evidence of the usefulness of HCC surveillance in high risk groups. It is important to establish public policies for HCC surveillance to improve the prognosis of patients in high risk groups for HCC development.
Notes
Authors’ contributions
W Sohn, D Kang, J Cho, and YH Paik have full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: W Sohn, J Cho, and YH Paik. Data acquisition: D Kang and M Kang. Data analysis and interpretation: W Sohn, D Kang, E Guallar, J Cho, and YH Paik. Drafting of the manuscript: W Sohn, D Kang, J Cho, and YH Paik. Critical revision of the manuscript for important intellectual content: M Kang and E Guallar. Statistical analysis: D Kang, M Kang, and J Cho. Financial support: YH Paik.
Conflicts of Interest
The authors have no conflicts to disclose.
Acknowledgements
This study was supported by The Research Supporting Program of the Korean Association for the Study of the Liver and The Korean Liver Foundation (KASLNHIS2017-001). This study used National Health Insurance Service (NHIS) data (NHIS-2018-4-056) from the Korean NHIS.
SUPPLEMENTAL MATERIAL
Supplementary material is available at Clinical and Molecular Hepatology website (http://www.e-cmh.org).
Subgroup analysis for all-cause mortality in patients with hepatocellular carcinoma (n=74,433). HR, hazard ratio; CI, confidence interval; HBV, hepatitis B virus.
Proportion of patients with the HCC surveillance by years. HCC, hepatocellular carcinoma.
Liver-related mortality in chronic liver disease according to HCC surveillance (n=1,209,825)
All-cause mortality among HCC patients according to surveillance
Effect of HCC surveillance on mortality among HCC patients after adjusting lead time bias
Abbreviations
AFP
alpha-fetoprotein
CCI
Charlson comorbidity index
CHB
chronic hepatitis B
CHC
chronic hepatitis C
CI
confidence interval
CT
computed tomography
HBV
hepatitis B virus
HCC
hepatocellular carcinoma
HCV
hepatitis C virus
HR
hazard ratio
ICD-10
International Classification of Diseases
IRB
Institutional Review Board
MRI
magnetic resonance imaging
NHIS
National Health Insurance Service
NLCSP
National Liver Cancer Screening Program
OR
odds ratio
RFA
radiofrequency ablation
References
Article information Continued
Notes
Study Highlights
• The Korea national screening program performs ultrasonography and serum AFP as HCC surveillance in chronic liver disease.
• HCC surveillance is effective in increasing the opportunity for curative treatment of HCC, and is associated with reduced in mortality among patients with chronic hepatitis B, chronic hepatitis C, or liver cirrhosis.
• HCC surveillance improves the prognosis of patients at high-risk for HCC development.