| Clin Mol Hepatol > Volume 25(3); 2019 > Article |
|
ABSTRACT
Background/Aims
Methods
FOOTNOTES
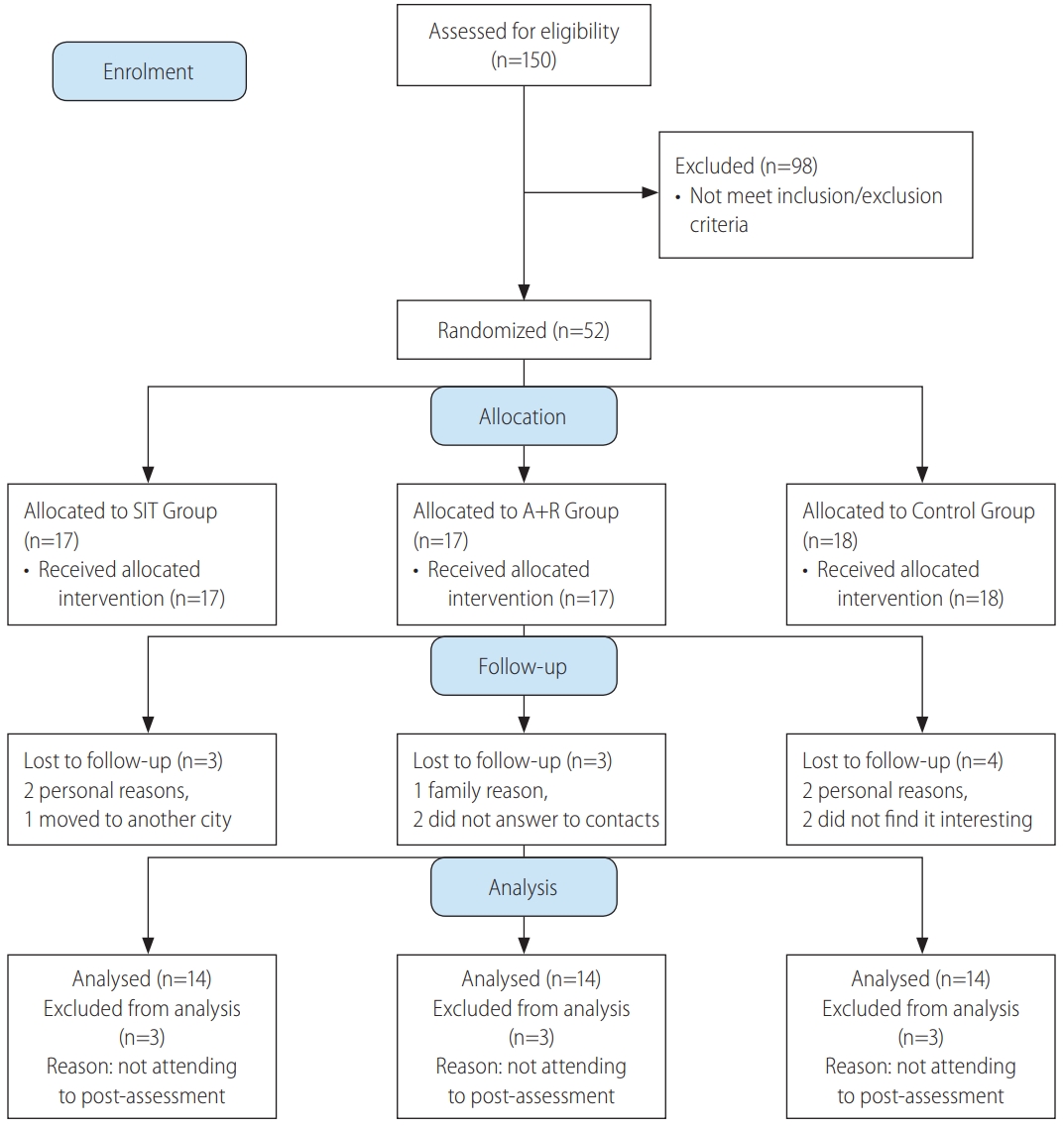
Figure┬Ā1.
Table┬Ā1.
Table┬Ā2.
Values are presented as mean┬▒standard deviation unless otherwise indicated. Twenty participants who used insulin were excluded from homeostasis model assessment of insulin resistance (HOMA-IR) analyses.
A+R training, aerobic and resistance training; BMI, body mass index; FBG, fasting blood glucose; HbA1c, hemoglobin A1c; AST, aspartate transaminase; ALT, alanine transaminase; GGT, gamma-glutamyl transferase; FLI, fatty liver index; FL, fatty liver; FSI, Framingham Steatosis Index; HSI, hepatic steatosis index; LAP, lipid accumulation product.
Table┬Ā3.
| SIT Group | A+R Group | Control Group | Time P-value | Time├ŚGroup P-value | |
|---|---|---|---|---|---|
| AST (IU/L) | 0.001 | 0.005 | |||
| ŌĆāPre | 6.93┬▒2.27 | 5.93┬▒1.54 | 9.29┬▒3.53 | ||
| ŌĆāPost | 9.21┬▒2.08 | 8.71┬▒2.58 | 8.50┬▒2.10 | ||
| ŌĆāP-value | 0.006 | 0.006 | 0.352 | ||
| ALT (IU/L) | 0.011 | 0.582 | |||
| ŌĆāPre | 3.93┬▒1.94 | 3.57┬▒2.28 | 4.36┬▒1.78 | ||
| ŌĆāPost | 4.92┬▒2.09 | 5.21┬▒2.33 | 5.07┬▒2.84 | ||
| ŌĆāP-value | 0.093 | 0.020 | 0.468 | ||
| AST/ALT ratio | 0.091 | 0.722 | |||
| ŌĆāPre | 1.96┬▒0.68 | 1.87┬▒0.99 | 1.94┬▒0.52 | ||
| ŌĆāPost | 2.66┬▒0.98 | 1.93┬▒0.81 | 2.04┬▒0.76 | ||
| ŌĆāP-value | 0.002 | 0.810 | 0.759 | ||
| GGT (IU/L) | 0.294 | 0.486 | |||
| ŌĆāPre | 16.24┬▒5.45 | 16.88┬▒4.87 | 18.61┬▒5.64 | ||
| ŌĆāPost | 13.78┬▒5.67 | 15.82┬▒4.75 | 18.47┬▒4.49 | ||
| ŌĆāP-value | 0.188 | 0.574 | 0.922 | ||
| FLI | <0.001* | 0.593 | |||
| ŌĆāPre | 62.17┬▒21.93 | 65.71┬▒14.19 | 59.94┬▒15.78 | ||
| ŌĆāPost | 42.39┬▒19.00 | 56.98┬▒21.45 | 48.78┬▒22.19 | ||
| ŌĆāP-value | 0.001 | 0.103 | 0.428 | ||
| FSI | 0.276 | 0.424 | |||
| ŌĆāPre | -0.35┬▒0.81 | -0.50┬▒0.63 | -0.54┬▒0.75 | ||
| ŌĆāPost | -0.84┬▒0.62 | -0.58┬▒0.65 | -0.80┬▒0.80 | ||
| ŌĆāP-value | 0.014 | 0.149 | 0.541 | ||
| HSI | <0.001* | 0.832 | |||
| ŌĆāPre | 38.10┬▒3.00 | 38.21┬▒5.32 | 37.61┬▒3.85 | ||
| ŌĆāPost | 37.80┬▒3.57 | 39.70┬▒8.87 | 37.51┬▒4.79 | ||
| ŌĆāP-value | 0.774 | 0.513 | 0.871 | ||
| LAP | <0.001* | 0.091 | |||
| ŌĆāPre | 85.45┬▒36.49 | 63.11┬▒10.26 | 74.69┬▒28.23 | ||
| ŌĆāPost | 48.01┬▒12.91 | 44.59┬▒10.53 | 61.77┬▒16.87 | ||
| ŌĆāP-value | 0.001 | 0.153 | 0.001 |
Values are presented as mean┬▒standard deviation unless otherwise indicated. Twenty participants who used insulin were excluded from homeostasis model assessment of insulin resistance (HOMA-IR) analyses.
A+R training, aerobic and resistance training; AST, aspartate transaminase; ALT, alanine transaminase; GGT, gamma-glutamyl transferase; FLI, fatty liver index; FSI, Framingham Steatosis Index; HSI, hepatic steatosis index; LAP, lipid accumulation product.
Table┬Ā4.
| SIT Group | A+R Group | Control Group |
P-values |
||
|---|---|---|---|---|---|
| Between Groups | Time├ŚGroup | ||||
| Weight (kg) | 0.024* | 0.477 | |||
| ŌĆāPre | 77.35┬▒11.99 | 72.59┬▒11.48 | 76.30┬▒9.59 | ||
| ŌĆāPost | 77.01┬▒12.35 | 72.34┬▒11.39 | 75.55┬▒9.23 | ||
| ŌĆāP-value | 0.372 | 0.438 | 0.483 | ||
| BMI (kg/m2) | 0.011* | 0.434 | |||
| ŌĆāPre | 29.27┬▒3.00 | 28.68┬▒4.34 | 30.12┬▒3.52 | ||
| ŌĆāPost | 29.14┬▒3.12 | 28.59┬▒4.35 | 29.82┬▒3.37 | ||
| ŌĆāP-value | 0.368 | 0.689 | 0.289 | ||
| BF % | 0.324 | 0.201 | |||
| ŌĆāPre | 41.14┬▒4.34 | 42.57┬▒2.17 | 42.64┬▒4.95 | ||
| ŌĆāPost | 42.64┬▒2.24 | 41.43┬▒4.18 | 44.50┬▒2.17 | ||
| ŌĆāP-value | 0.041 | 0.291 | 0.379 | ||
| FBG (mg/dL) | <0.001* | 0.034* | |||
| ŌĆāPre | 210.07┬▒32.90 | 214.64┬▒27.67 | 200.86┬▒46.88 | ||
| ŌĆāPost | 137.36┬▒32.95 | 163.86┬▒71.47 | 190.50┬▒59.71 | ||
| ŌĆāP-value | 0.001 | 0.039 | 0.690 | ||
| Insulin (╬╝U/mL) | 0.019* | 0.468 | |||
| ŌĆāPre | 10.08┬▒5.43 | 10.37┬▒5.35 | 9.55┬▒4.05 | ||
| ŌĆāPost | 8.18┬▒5.75 | 8.83┬▒7.60 | 9.16┬▒3.75 | ||
| ŌĆāP-value | 0.001 | 0.001 | 0.082 | ||
| HbA1c (%) | <0.001* | 0.006* | |||
| ŌĆāPre | 9.64┬▒1.08 | 9.49┬▒0.86 | 9.10┬▒0.51 | ||
| ŌĆāPost | 7.82┬▒0.93 | 8.25┬▒1.22 | 9.12┬▒1.41 | ||
| ŌĆāP-value | 0.001 | 0.002 | 0.643 | ||
| HOMA-IR | 0.093 | 0.288 | |||
| ŌĆāPre | 3.51┬▒1.97 | 2.28┬▒0.42 | 2.84┬▒0.99 | ||
| ŌĆāPost | 3.72┬▒1.17 | 3.66┬▒1.24 | 3.01┬▒1.89 | ||
| ŌĆāP-value | 0.001 | 0.001 | 0.734 | ||
Values are presented as mean┬▒standard deviation unless otherwise indicated. Twenty participants who used insulin were excluded from homeostasis model assessment of insulin resistance (HOMA-IR) analyses.
A+R training, aerobic and resistance training; BMI, body mass index; BF %, body fat percent; FBG, fasting blood glucose; HbA1c, hemoglobin A1c.
Abbreviations
REFERENCES
- TOOLS
-
METRICS

- ORCID iDs
-
Ebrahim Banitalebi

https://orcid.org/0000-0002-9943-9747 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



