| Clin Mol Hepatol > Volume 23(4); 2017 > Article |
|
ABSTRACT
Figure 1.
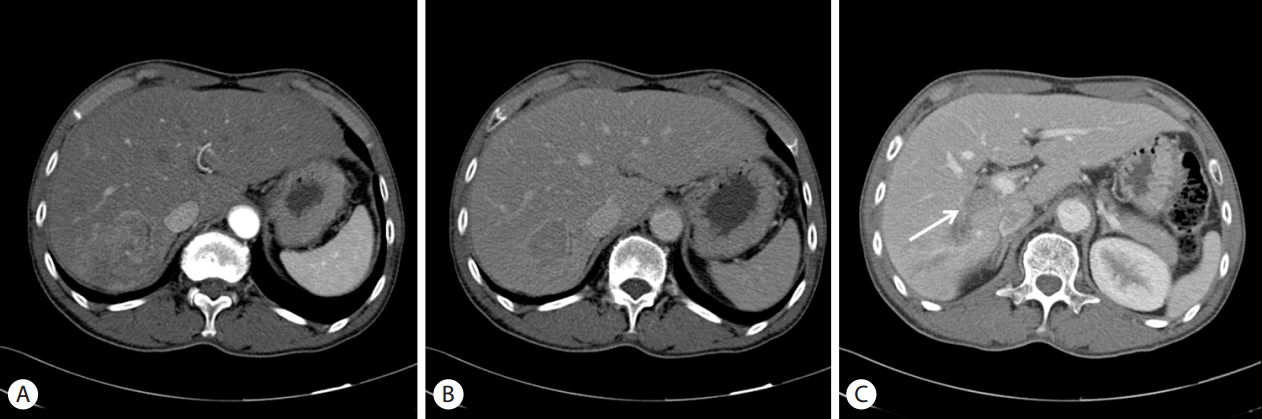
Figure 2.
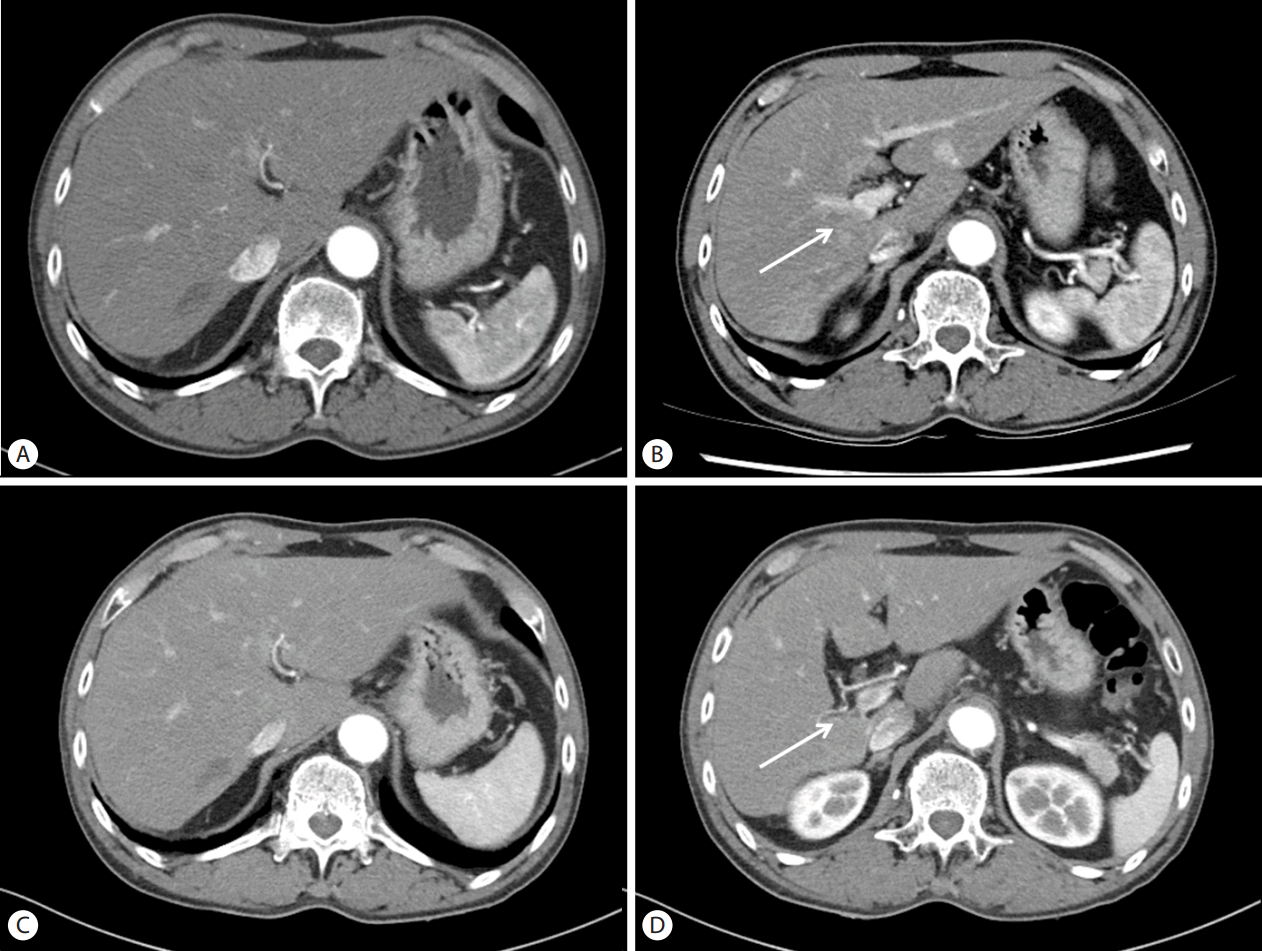
Figure 3.
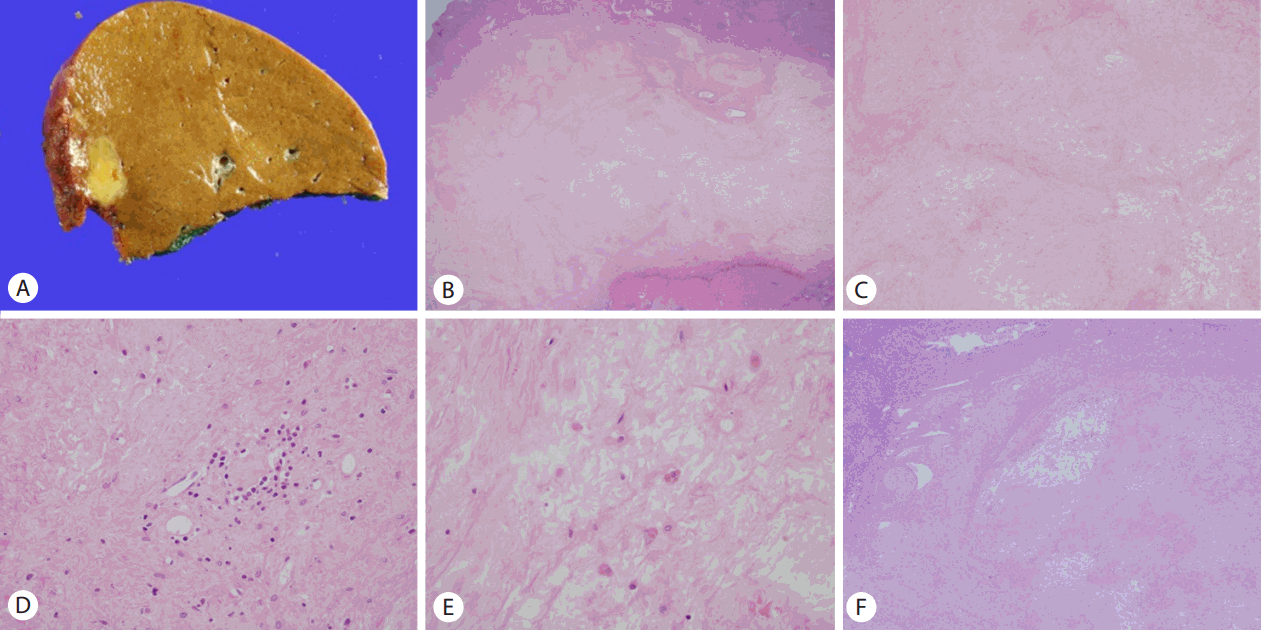
Table 1.
|
Intrahepatic tumor |
|||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Published | Characteristics | Etiology | Metastasized to | Max diameter (cm) | Initial dose (mg/day) | Time to CR (mon) | Time to cessation (mon) | Histologic CR | Initial AFP (ng/mL) | PVTT | F/u period (mon) | Bx. at diagnosis | Child-Pugh class | HFSR | HCC related treatment |
| So et al. [9] (2008) | 78, M, USA | HHC | Lung | Multiple | 800 | 5 | 6 | NA | 13,599 | Unknown | 6 | diagnosis | Pugh | No | - |
| 5.0 | class | ||||||||||||||
| Yeganeh et al. [10] (2009) | 54, M, USA (Asian) | HBV | Lung (4.1 cm) | No | 800 | 18 | Maintain | NA | 1.3 | No | Unknown | No | Unknown | Yes | RFA, TACE, OLT, Adjuvant chemotherapy |
| - | |||||||||||||||
| Wang et al. [11] (2010) | 74, M, USA | HCV | - | Single | 400 | 8 | 8 | NA | 3300 | Yes | 19 | No | A | Unknown | - |
| 10 | |||||||||||||||
| Kudo et al. [12] (2010) | 68, M, Japan | HBV | Lung | Single | 800 | 2 | Unknown | NA | 18,775 | Invasion to | >1 year | No | A | Unknown | TACE |
| Unknown | IVC | ||||||||||||||
| Kudo et al. [12] (2010) | 68, M, Japan | HBV | Lung, lymph node, adrenal gland | Multiple | 400 | 6 | Maintain | NA (Metastatic lesion) | 10,559 | Yes | >1 year | No | A | Unknown | TACE, Hepatectomy, HAIC |
| Unknown | |||||||||||||||
| Chelis et al. [13] (2011) | 69, M, Greece | HBV+HIV | Lymph node | Single | 400 | 6 | Unknown | NA | W.N.L | Unknown | 10 | Yes | Unknown | Yes | TACE HARRT |
| 5.2 | |||||||||||||||
| Sacco et al. [14] (2011) | 84, M, Italy | HCV | - | Single | 800 | 6 | Maintain | NA | 353 | Yes | 12 | No | A | No | - |
| 6.0 | |||||||||||||||
| Curtit etal. [15] (2011) | 56, M, France | HCV | Diaphragm, IVC | Multiple | 800 | 6 | 6 | Yes | 3,315 | No | 6 | No | A | Yes | Surgical resection |
| 15 | |||||||||||||||
| Irtan et al. [16] (2011) | 59, M, France | HHC | Lymph node, omentum | Single | 800 | 6 | 6 | Yes | 效 6 | Yes | 16 | No | A | Yes | Surgical resection |
| 10 | |||||||||||||||
| Irtan et al. [16] (2011) | 57, M, France | HBV | - | Single | 800 | 12 | 12 | Yes | 17,000 | Yes | 12 | No | A | No | Surgical resection |
| 8 | |||||||||||||||
| Inuzuka et al. [8] (2011) | 76, F, Japan | HCV | Lung (>60) | No | 400 | 4 | 4 | NA | 6,952 | No | 8 | No | A | No | PEI, TACE, RFA |
| - | |||||||||||||||
| Mizukami et al. [17](2012) | 69, M, Japan | HCV | Lymph node | No | 800 | 0.4 | 0.4 | NA | 25.1 | No | 10 | No | A | Yes | - |
| - | |||||||||||||||
| Kim et al. [18] (2013) | 66, M, Korea | Alcoholic | Lymph node | Multiple | 800 | 3 | 12 | NA | 2,795 | Yes | 8 | No | A | Unknown | TACE, HAIC |
| LC | Unknown | ||||||||||||||
| Kermiche-Rahali et al. [19] (2013) | 68, M, France | Alcoholic | - | Single | 800 | 10 | 9 | Yes | 9效 | No | 14 | No | A | Yes | Surgical resection |
| LC | 15.7 | ||||||||||||||
| Moroni et al. [20] (2013) | 78, M, Italy | HCV | - | Single | 800 | 22 | 22 | NA | 58,560 | Yes | 26 | Yes | A | Yes | |
| 9.0 |
AFP, alpha-fetoprotein; CR, complete response; PVTT, portal vein tumor thrombosis; HFSR, hand-foot skin reaction; HCC, hepatocellular carcinoma; HHC, hereditary hemochromatosis;; HBV, hepatitis B virus; HCV, HCV, hepatitis C virus; HIV, human immunodeficiency virus; LC, liver cirrhosis; IVC, inferior vena cava; RFA, radiofrequency ablation; TACE, transarterial chemoembolization; PEI, percutaneous ethanol injection; OLT, orthotopic liver transplantation; HAIC, hepatic arterial infusion chemotherapy; HAART, Highly Active Antiretroviral Therapy; NA, Not available.
Abbreviations
REFERENCES
- TOOLS
-
METRICS

- ORCID iDs
-
Ji Hoon Kim

https://orcid.org/0000-0003-3924-0434 - Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



